Chapter 4 – Communicating (2nd Ed.)
(This Chapter comes from the 2003 2nd Edition of the book and has been expanded and updated in the 2015 3rd edition, with new sections to cover topics including interruptions and clinical handover)
Every clinical action, every treatment choice and investigation, is shaped by the available information. We can think of this information as the clinical evidence that is used to make a judgement about the right course of action. Clinicians gather evidence through communication with others, either through what is said now, or what has been documented from before.
There are many different sources of clinical evidence that can be used in the routine care of a patient, and these include:
· The patient, who will give information about their symptoms and their problems, as well as demonstrate clinical signs through physical examination,
· The clinical literature, which captures past knowledge about disease and treatment,
· The patient record, which records the history of a patient’s state, both based upon clinical observation and laboratory and imaging reports, as well as their various treatments and the impact of treatment on their disease,
· Clinical measurement devices, from the simple like a blood pressure cuff, through to the complex such as a glucometer, cardiogram or multi-probe patient monitor in intensive care,
· Clinical colleagues, who may exchange messages containing information about the state of patients, their opinions, their own workload and needs, or clinical knowledge.
The information contained in these clinical “messages” comes in a variety of media and formats and can be delivered in a variety of ways including face-to-face conversations, letters, e-mail, voicemail, and electronic or paper medical records.
When this exchange of information works well, clinical care is solidly based upon the best evidence. When information exchanges are poor, the quality of clinical care can suffer enormously. For example, the single commonest cause of adverse clinical events is medication error, which account for about 19% of all adverse events, and the commonest prescription errors can be redressed by the provision of better information about medications or the patients receiving them (Bates et al, 2001). Poor presentation of clinical data can also lead to poorly informed clinical practice, inappropriate repeat investigation, unnecessary referrals, and wastes clinical time and other resources (Wyatt and Wright, 1998).
In this chapter we will look at the communication process and explore how variations in the structure of clinical messages affect the way in which they are interpreted, and therefore affect the quality of care. If the motto for Chapter One was “A map is not the territory” then the motto for this Chapter is “the chart is not the patient”.
4.1 The structure of a message determines how it will be understood
What a message is meant to say when it is created, and what the receiver of a message understands, may not be the same. This is because what humans understand is profoundly shaped by the way data are presented to us, and by the way we react to different data presentations. Thus it is probably as important to structure data in a way so that it can be best understood, as it is to ensure that the data are correct in the first place.
What a clinician actually understands after seeing the data in a patient record and what the data actually shows are very different things. For example, the way data are structured has a profound effect on the conclusions a clinician will draw from the data. In Figure 4.1, identical patient data are presented in four different ways (Elting et al., 1999). The data show preliminary results from two hypothetical clinical trials of a generic “conventional treatment” compared with a generic “investigational treatment”, both treating the same condition. In an experiment to see if clinicians would decide to stop the trial because the data show one of the treatments was obviously better than the other, the decision to stop varied significantly depending upon how the data were displayed. Correct decisions were significantly more common with icon displays (82%) and tables (68%) than with pie charts or bar graphs, both 56%.
If this example was reflected in actual clinical practice, up to 25% of the patients treated according to data displayed as bar or pie charts would have received inappropriate treatment. Consequently, there is an enormous difference between simply communicating a message to a colleague, and communicating it effectively.
4.2 The message that is sent may not be the message that is received
Messages are misunderstood both because of the limitations of the agents interpreting them, and because the very process of communication itself is limited. To explore the nature of communication, we will develop a general model that describes the process of sending a message between two agents. The agents might be two human beings, or a human and a computer. A communication act occurs between the two agents A1 and A2 when agent A1 constructs a message m1 for some specific purpose, and sends m1 to agent A2 across a communication channel.
The second agent A2 receives a message m2, which may in some ways be different from the intended message m1. The effectiveness of the communication between the agents is dependent upon several things – the nature of the channel, the state of the individual agents, the knowledge possessed by the agents, and the context within which the agents find themselves.
Communication channels distort messages
A wide variety of different communication channels are available to us, from the basic face-to-face conversation, through to telecommunication channels like the telephone or e-mail, and non-interactive channels like the medical record.
The message is sent as a signal down the channel, and the message signal may be corrupted because of limitations in the channel bearing the message. For example, faxed or photocopied documents may be harder to read than digitally transmitted documents because of poor resolution and distortion of the transmitted document.
Channels vary in their capacity to carry data, and the more limited the channel capacity, the less of the original message can be transmitted at any one time. Simply put, the thinner the channel ‘pipe’, the less data can flow through at any given moment.
| The signal to noise ratio measures how much a particular message has been corrupted by noise that has been added to it during transmission across a channel. |
Channels also have different abilities to send a message exactly as it was sent, and often the message is distorted in transmission. This distortion is usually called noise. Noise can be thought of technically as any unwanted signal that is added to a transmitted message while being carried along a channel, and distorts the message for the receiver. So, noise can be anything from the static on a radio, to another conversation next to your own, making it hard to hear your partner – one person’s signal is another’s noise. Standard information theory describes how the outcome of a communication is determined in part by the capacity and noise characteristics of a channel (see Box 4.1).
So, we note that in general, when an agent sends a message, the message may be modified by the channel, and be received as a slightly different message by the receiving agent.
Individuals don’t know the same things
In Chapter two we saw that the inferences that can be drawn from data are dependent on the knowledge used to make the inference. Since different individuals ‘know’ slightly different things, they will usually draw different inferences from the same data because of this variation in their individual knowledge. Thus variations in diagnosis and treatment decisions, based upon the same data, may simply reflect the differences in clinical knowledge between individual clinicians.
However, when sending a message, we have to make assumptions about the knowledge that the receiver has, and use that to shape our message. There is no point in explaining what is already known, but it is equally as important to not miss out important details that the receiver should know to draw the right conclusions. Thus notionally identical messages sent to a clinical colleague or to a patient end up being very different because we assume that the colleague has more common knowledge, and requires less explanation, than the patient. The knowledge shared between individuals is sometimes called common ground (Coiera, 2000).
This explains why individuals communicate more easily with others that have similar experiences, beliefs and knowledge. Intuitively we know that it takes greater effort to explain something in a conversation to someone with whom we share less common background. Conversely, individuals who are particularly close can communicate complicated ideas in terse shorthand. One of the reasons agents create common ground is to optimise their interaction. By sharing ground, less needs to be said in any given message, making the interaction less costly (Box 21.1).
With this in mind, we can now say that each agent possesses knowledge about the world, in the form of a set of models K. Critically, the private world models of the two communicating agents in our model, K1 and K2, are not identical. Thus agent A1 creates a message m1, based upon its knowledge of the world K1 (Figure 4.2). A2 receives a slightly different message m2 because of channel effects, and then generates its own private interpretation of the message’s meaning based upon its own knowledge K2. Further, agent A1 makes a guess about the content of K2, and shapes its message to include data or knowledge it believes agent A2will need to make sense of the message being sent. The effectiveness of the message is dependent upon the quality of the guess an agent can make about what the receiving agent knows. Usually, agents send more than is needed, because some redundancy in a message improves the chance that what the receiver needs is actually sent.

| Figure 4.2: When a message is sent between two agents, it is built according to a model that we think will be understood by the receiving agent, and is potentially distorted during transmission by the communication channel. |
Messages are constructed according to imperfect models of the world
Sending and receiving messages are model-based processes. Consequently, the process of communication is fundamentally limited in its capacity not just by physical limitations of transmission channels, but by the inherent limitations of modelling which were outlined in Chapter one.
Model theory tells us that the sender of a message is operating with models of the world that will always be inaccurate in one way or another, and that equally, the receiver must attempt to interpret messages according to models that are themselves flawed in some way. Consequently, communication will never be a perfect process, and misinterpretation is at some level unavoidable.
The process of human communication suffers from some specific limitations that arise from the way humans use models, either to interpret physical symbols from data received by the senses, or to interpret that sense data according to mental models of the world:
| Figure 4.3: The Müller-Lyer illusion demonstrates how human perception distorts sense data. The central lines in both upper and lower figures are actually identical in length, but the lower segment appears to be longer. |
· Perceptual limitations –We may misperceive the symbols that have been written or said to us. This may simply occur when the symbols are poorly constructed and therefore ambiguous. Drug names are often confused because of illegible handwritten script. Further, each of the human senses can be thought of as a communication channel, each with its own unique capacities to carry and distort data. For example, individuals have different abilities to hear or see, and messages may be misunderstood because of sensory deficits. However, at a more fundamental level, the human perceptual system itself distorts sense data, exaggerating some characteristics and minimizing others. It does this presumably because the brain has evolved to preferentially recognise some patterns over others as more important to survival. Consequently, what we perceive, and what actually is, are not the same thing (Figure 4.3). Although there is much argument about the exact process, perception is an active process of attempting to map sense data to internal models of the world (Van Leeuwen, 1998). Humans often try and fit what we sense through sight, sound, touch and smell to our pre-existing models of what we think should be there (figure 4.4).
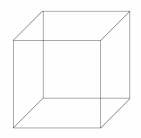
| Figure 4.4: There are two possible interpretations of this cube depending on whether you think the rightmost square surface is at the back or the front of the three dimensional cube. |
· Human attention limitations – Humans may not pay enough attention to a message, and miss some of its content, or misinterpret the content. This occurs because human attention has a very limited capacity to process items (see Box 8.1). When individuals are distracted by other tasks, they are less likely to have the capacity to fully attend to a message. So, when receiving a message, the amount of cognitive resource available to an individual determines the quality of the inferences they can draw. When a message is constructed, we should therefore consider the cognitive state of the individual receiving the message. For example, in a stressful situation, a clinical flowchart that makes all the steps in treating a patient explicit will require less attention than the same information presented as paragraphs of unstructured text, which require the reader to extract the appropriate steps in the treatment.
· Cognitive biases – Humans do not perceive information in a neutral way, but have an inherent set of biases that cause us to draw conclusions not supported by the immediate evidence (see Box 8.2). Put simply, we hear what we want to hear, or think we should hear. For example, recent events can bias us to recognize similar events, even when they are not present. Thus an encounter with a thyrotoxic patient can bias a clinician to overdiagnose the same disease in future underweight patients (Medin et al., 1982). Humans also react to positive information differently to negative information. The way in which treatment results were framed in the experiments shown in Figure 4.1 made a significant difference. Negatively framed tables (those reporting treatment failure rates) resulted in significantly more decisions to stop treatment than positive ones reporting success rates (Elting et al., 1999).
4.3 Grice’s conversational maxims provide a set of rules for conducting message exchanges
How is it that agents, whether they are human or computer, manage to communicate effectively given the inherent limitations of message exchange? More importantly from our point of view, given that poor communication can have a profound negative impact on health care delivery, what makes a good message?
One of the most influential answers to these questions comes from the work of H. Paul Grice (1975) who took a very pragmatic approach to the mechanics of conversation. Grice suggested that well-behaved agents all communicate according to a basic set of rules that ensure conversations are effective and that each agent understands what is going on in the conversation.
Most generally, the cooperative principle asks each agent that participates in a conversation to do their best to make it succeed. Agents should only make appropriate contributions to a conversation, saying just what is required of them, saying it at the appropriate stage in the conversation, and only to satisfy the accepted purpose of the conversation. Grice proposed a set of four maxims, which explicitly defined what he meant by the principle of co-operation:
1. Maxim of Quantity: Say only what is needed.
1.1. Be sufficiently informative for the current purposes of the exchange.
1.2. Do not be more informative than is required.
2. Maxim of Quality: Make your contribution one that is true.
2.1. Do not say what you believe to be false.
2.2. Do not say that for which you lack adequate evidence.
3. Maxim of Relevance: Say only what is pertinent to the context of the conversation at the moment.
4. Maxim of Manner:
4.1. Avoid obscurity of expression.
4.2. Avoid ambiguity.
4.3. Be brief.
4.4. Be orderly.
There are some overlaps in the maxims, but they do lay out a set of rules that guide how conversations should proceed. Clearly also, people do not always follow these maxims. Sometimes it is simply because agents are not well behaved. At other times, agents break the rules on purpose to communicate more subtle messages. For example, people are often indirect in their answers when asked a question. If someone asked you “How much do you earn?’ a wry answer might be “Not enough!” or something similarly vague. Such an answer clearly is uncooperative, and violates the maxim of quantity, relevance, and manner in different ways. However, the clear message behind the answer is “This is none of your business.” The intentional violation of maxims allows us to signal things without actually having to say them, either because it might be socially unacceptable, or because there are other constraints on what can be said at the time (Littlejohn, 1996).
4.4 Conclusions
In this chapter, we have used the idea of models and templates to develop a rich picture of the process of structuring and communicating information. Communication is a complex phenomenon that is usually ignored in routine clinical practice, yet getting it right has profound implications for the quality of patient care. In the next Chapter we are going to take this communication model and use it explain the ways we can structure one of commonest of clinical ‘messages’ – the patient record.
Box 4.1 – Information theory
Claude Shannon developed the mathematical basis for information theory while working at Bell Laboratories during the 1940s. Motivated by problems in communication engineering, Shannon developed a method to measure the amount of ‘information’ that could be passed along a communication channel between a source and a destination.
Shannon was concerned with the process of communicating using radio, and for him the transmitter, ionosphere and receiver were all examples of communication channels. Such channels had a limited capacity and were noisy. Shannon developed definitions of channel capacity, noise and signal in terms of a precise measure of what he called ‘information’.
He began by recognising that before a message could enter a channel it had to be encoded in some way by a transmitter. For example, a piece of music needs to be transformed through a microphone into electronic signals before it can be transmitted. Equally, a signal would then need to be decoded at the destination by a receiver before it can be reconstructed into the original signal. A hi-fi speaker thus needs to decode an electronic signal before it can be converted back into sound.
Shannon was principally interested in studying the problem of maximising the reliability of transmission of a signal, and minimising the cost of that transmission. Encoding a signal was the mechanism for reducing the cost of transmission through signal compression, as well as combating corruption of the signal through channel noise.
The rules governing the operation of an encoder and a decoder constitute a code. The code described by Shannon corresponds to a model and its language. A code achieves reliable transmission if the source message is reproduced at the destination within prescribed limits. After Shannon, the problem for a communication engineer was to find an encoding scheme that made the best use of a channel while minimising transmission noise.
With human verbal communication, the information source is the sender’s brain and the transmitter is the vocal chords. Air provides the communication channel, and may distort any message sent because of extraneous noise, or because the message gets dampened or attenuated the further the distance between the communicating parties. The receiver in this model is the listener’s ear, and the destination that decodes what has been received is the listener’s brain. Although Shannon saw his theory helping us understand human communication, it remains an essentially statistical analysis over populations of messages, and says little about individual acts of communication. Specifically information theory is silent on the notion on the meaning of a message, since it does not explicitly deal with the way a knowledgebase is used to interpret the data in a message.
Further Reading:
J. C. A. van der Lubbe, Information Theory, Cambridge University Press, (1997).
Discussion Points
1. “The chart is not the patient”. Explain why people might confuse the two, perhaps thinking back to Chapter One, and explain why they should keep the two separate, perhaps thinking of the principles in this Chapter.
2. Marshall McLuhan famously said “the medium is the message”. What did he mean? Do you agree?
3. The way we interpret a message is shaped by the way a message is constructed. Give examples of the way public figures like politicians shape their messages to have a specific impact on public opinion.
4. A politician will shape their message differently, depending upon which medium they are using at the time. Compare the way the same message will look on television news, in the newspaper, in a magazine article, or when delivered over the phone or face-to-face.
5. In the game ‘Chinese whispers’ a message is passed along a chain, from one individual to the next. By the time the message reaches the end of the chain it is highly distorted compared to the original. Explain the possible causes of this message distortion.
6. Within healthcare, a message can be passed down long chains of individuals. What mechanisms do we have to prevent the ‘Chinese whispers’ effect distorting critical clinical data?
7. You need to send a copy of a 200-page paper medical record to a colleague in another institution. What is the best channel to use? Consider the impact that urgency, distance or cost might make on your answer.
8. You have a question about your patient’s treatment. What is the best channel to use to get an opinion from a colleague?
Chapter Four Summary
1. What a message is meant to say when it is created, and what the receiver of a message understands, may not be the same.
2. The structure of a message determines how it will be understood. The way clinical data can alter the conclusions a clinician will draw from the data.
3. The message that is sent may not be the message that is received. The effectiveness of communication between two agents is dependent upon:
· the communication channel which will vary in capacity to carry data and noise which distorts the message,
· the knowledge possessed by the agents, and the common ground between them,
· the resource limitations of agents including cognitive limits on memory and attention,
· the context within which the agents find themselves which dictate which resources are available and the competing tasks at hand.
4. Grice’s conversational maxims provide a set of rules for conducting mesasage exchanges:
4.1. Maxim of Quantity: Say only what is needed.
4.2. Maxim of Quality: Make your contribution one that is true.
4.3. Maxim of Relevance: Say only what is pertinent to the context of the conversation at the moment.
4.4. Maxim of Manner: Avoid obscurity of expression, ambiguity, be brief and orderly.
© Enrico Coiera 2003-2014




Leave a comment